Attention Deficit Hyperactivity Disorder (ADHD) has become one of the most common neurodevelopmental and psychiatric disorders of childhood (3% to 7% of school-age children), that persists to adolescence and adulthood in 40-60% cases. ADHD treatment main strategies are the use of pharmacological therapy, omega 3, multivitamins, and multi-minerals. Stimulants work by causing the brain to synthesize more norepinephrine; non-stimulants by slowing the rate at which norepinephrine is broken down. Once the level is where it should be, the brain functions normally, and the individual becomes less hyperactive, inattentive, and/or impulsive. Once the drug wears off, the level falls — and symptoms return. In addition, side-effects, resistance to pharmacological therapy have raised interest in non-pharmacological treatment options. Neurofeedback for ADHD management is a non-pharmacological intervention, based on neuroplasticity characteristics of the brain and utilizes cognitive behavioral therapeutic elements to gain access on and practice brain activity. In fact, several organizations worldwide are looking into claims that neurofeedback such effective as pharmacological therapy, but with significantly long-lasting effectiveness and free of side-effects. This became more actual if take into consideration existing today friendly use technology of neurofeedback devices for ADHD management at home, school, university, and workplace.
Attention-deficit hyperactivity disorder (ADHD) is the most commonly diagnosed behavioral disorder in children, but it is often misunderstood as well as the subject of controversy. Confusion surrounding the disorder has led to both under- and overtreatment of children. Currently, the disorder is primarily diagnosed by referring to the criteria of the Diagnostic and Statistical Manual of Mental Disorders-Fourth Edition Text Revision (DSM-IV, 1994) or the International Statistical Classification of Mental Disorders (ICD-10, World Health Organization, 1992).
Attention-deficit/hyperactivity disorder (ADHD) is a childhood-onset, clinically heterogeneous disorder of inattention, hyperactivity, and impulsivity. Its impact on society is enormous in terms of its financial cost, stress to families, adverse academic and vocational outcomes, and negative effects on self-esteem. Children with ADHD are easily recognized in clinics, in schools, and in the home. Their inattention leads to daydreaming, distractibility, and difficulties in sustaining effort on a single task for a prolonged period. Their impulsivity makes them accident-prone, creates problems with peers, and disrupts classrooms. Their hyperactivity, often manifested as fidgeting and excessive talking is poorly tolerated in schools and is frustrating to parents, who can easily lose them in crowds and cannot get them to sleep at a reasonable hour. In their teenage years, symptoms of hyperactivity and impulsivity diminish, but in most cases, the symptoms and impairments of ADHD persist. The teen with ADHD is at high risk of low self-esteem, poor peer relationships, conflict with parents, delinquency, smoking, and substance abuse.
The validity of diagnosing ADHD in adults has been a source of much controversy. Some investigators argue that most cases of ADHD remit by adulthood (3), a view that questions the validity of the diagnosis in adulthood. Others argue that the diagnosis of ADHD in adults is both reliable and valid.
Longitudinal studies have found that as many as two-thirds of children with ADHD have impaired ADHD symptoms as adults. In adults, inner restlessness rather than hyperactivity may occur. Throughout the life cycle, a key clinical feature observed in patients with ADHD is comorbidity with conduct, depressive, bipolar, and anxiety disorders.
ADHD Symptoms in Children and Teenagers
ADHD is divided into three subtypes:
- predominantly inattentive (ADHD-PI or ADHD-I),
- predominantly hyperactive-impulsive (ADHD-PH or ADHD-HI), and
- combined type (ADHD-C).
The symptoms of ADHD in children and teenagers are well-defined, and they’re usually noticeable before the age of 6. They occur in more than one situation, such as at home and school.
Inattentiveness
The main signs of inattentiveness are:
• having a short attention span and being easily distracted
• making careless mistakes – for example, in schoolwork
• appearing forgetful or losing things
• being unable to stick to tasks that are tedious or time-consuming
• appearing to be unable to listen to or carry out instructions
• constantly changing activity or task
• having difficulty organizing tasks
Hyperactivity and impulsiveness
The main signs of hyperactivity and impulsiveness are:
• being unable to sit still, especially in calm or quiet surroundings
• constantly fidgeting
• being unable to concentrate on tasks
• excessive physical movement
• excessive talking
• being unable to wait their turn
• acting without thinking
• interrupting conversations
• little or no sense of danger
These symptoms can cause significant problems in a child’s life, such as underachievement at school, poor social interaction with other children and adults, and problems with discipline.
A common symptom of ADHD in children and adults is the inability to focus at length on the task at hand. Those who have ADHD are easily distracted, which makes it difficult to give sustained attention to a specific activity, assignment, or chore. But a lesser-known, and more controversial, symptom that some people with ADHD demonstrate is known as hyperfocus. Although other conditions include hyperfocus as a symptom, here we will look at hyperfocus as it relates to a person with ADHD.
Hyperfocus is the experience of intense concentration in some people with ADHD. ADHD is not necessarily a deficit of attention, but rather a problem with regulating one’s attention span to desired tasks. So, while mundane tasks may be difficult to focus on, others may be completely absorbing. An individual with ADHD who may not be able to complete homework assignments or work projects may instead be able to focus for hours on video games, sports, or reading.
People with ADHD may immerse themselves so completely in an activity that they want to do or enjoy doing to the point that they become oblivious to everything around them. This concentration can be so intense that an individual loses track of time, other chores, or the surrounding environment. While this level of intensity can be channeled into difficult tasks, such as work or homework, the downside is that ADHD individuals can become immersed in unproductive activities while ignoring pressing responsibilities. No one’s going to mind if someone spends hours solving math problems or painting the house. But hyperfocus can cause trouble if someone gets so wrapped up in a project at work that misses a dinner date, or the child can’t break away from a video game to do his homework.
It also can make it harder to diagnose ADHD, especially in kids considered gifted. They do better in school because their high IQs help them get past the learning issues that usually go along with the disorder, and their ability to hyperfocus can make it even harder to spot.
It is very important to find ways to manage the focus of children with ADHD and direct it for their development and good performance, finding an interest that removes them from isolated time and fosters social interaction, such as music, sports, or other.
Adults with ADHD also have to deal with hyperfocus, on the job, and at home. The best way to cope with hyperfocus is not to fight it by forbidding certain activities, but rather to harness it. Making work or school stimulating can capture their focus in the same way as their favorite activities. This may be difficult for a growing child but can ultimately become advantageous for an adult in the workplace. By finding a job that caters to one’s interests, an individual with ADHD can truly shine, using hyperfocus to their advantage.
If you’re a parent of a child with attention deficit hyperactivity disorder, you know that their attention can be directed quite intensely onto technology they find fascinating, which includes cell phone games, texting, the internet, and social media. These facets of mobile phone use provide an endless supply of feedback and enticements that keep the pleasure center of the brain very happy, which can make pulling a child away from their phone or yours a real struggle.
Though researchers do not yet know whether excessive phone use increases the risk of ADHD, encouraging thoughtful and limited cell phone use is considered an important life skill for any child. However, there is a correlation between ADHD and high levels of cell phone use, and the increase in children diagnosed with the disorder make researchers wonder how the rise of mobile technology impacts the attention levels of young children and teens. One study found that children who make calls and play games on cell phones were at increased risk for ADHD. However, it is possible that children may play more games on their phone because they already have symptoms of ADHD, such as inattention and hyperfocus.
Some children can become engrossed with a particular smartphone game or app and later toss it aside, but kids with ADHD are at higher risk for becoming behaviorally and cognitively dependent on their device. This can be a cause for concern, as researchers have linked cell phone dependence to symptoms of anxiety, depression, sleep disturbances, and low self-esteem.
Being dependent or overinvolved with a cell phone isn’t just about the number of games a child plays or the texts they send. Kids with ADHD can become caught in a behavioral loop, mindlessly checking different social media apps or seeking to achieve the reach level in a difficult game. Dependence has a cognitive component as well, with the child thinking about or becoming hyperfocused on being able to access and use their phone. For example, they might become distressed when the battery dies, when their phone is not in sight, or when they cannot sleep with their cell phone at night.
Although hyperfocus can have a detrimental effect on a person’s life by distracting them from important tasks, it can also be used positively, as evidenced by many scientists, artists, and writers. Like all symptoms of ADHD, hyperfocus needs to be delicately managed.
When in a hyperfocused state, a child may lose track of time and the outside world may seem unimportant.
It is very important to find ways to manage the focus of children’s with ADHD and direct it for their development and good performance. First of all, for parents, it is necessary to monitor the length of use and the content accessed on their child’s phone and to keep mobile devices out of a child’s bedroom to ensure healthy sleep habits. Less phone use won’t feel like a punishment if kids and teens have flexible, fun options when it comes to their attention. What activities does your child enjoy that don’t involve screens, and how can they be utilized when your child seems particularly dependent on their phone? A day at the park, a museum, or the pool can prove a much-needed break in hyper-focus. Help your child find an interest that removes them from isolated time and fosters social interaction, such as music or sports.
Neurofeedback management of ADHD gives excellent results and leads to significant improvement of memory, attention, concentration, and focus. These improvements will provide the possibility to stop addiction to phones and computers.
Video – More screen tine leads to ADHD
Related conditions in children and teenagers with ADHD
Although not always the case, some children may also have signs of other problems or conditions alongside ADHD, such as:
• Anxiety disorder – which causes your child to worry and be nervous much of the time; it may also cause physical symptoms, such as a rapid heartbeat, sweating, and dizziness
• Oppositional defiant disorder (ODD) – this is defined by negative and disruptive behavior, particularly towards authority figures, such as parents and teachers
• Conduct disorder – this often involves a tendency towards highly antisocial behavior, such as stealing, fighting, vandalism, and harming people or animals
• Depression
• Sleep problems – finding it difficult to get to sleep at night, and having irregular sleeping patterns
• Autistic spectrum disorder (ASD) – this affects social interaction, communication, interests, and behavior
• Epilepsy – a condition that affects the brain and causes repeated fits or seizures
• Tourette’s syndrome – a condition of the nervous system, characterized by a combination of involuntary noises and movements (tics)
• Learning difficulties – such as dyslexia
ADHD Symptoms in Adults
In adults, the symptoms of ADHD are more difficult to define. This is largely due to a lack of research into adults with ADHD.
As ADHD is a developmental disorder, it’s believed it cannot develop in adults without it first appearing during childhood. However, it’s known that symptoms of ADHD often persist from childhood into a person’s teenage years and then adulthood.
Any additional problems or conditions experienced by children with ADHD, such as depression or dyslexia, may also continue into adulthood. By the age of 25, an estimated 15% of people diagnosed with ADHD as children still have a full range of symptoms, and 65% still have some symptoms that affect their daily lives. Hyperactivity tends to decrease in adults, while inattentiveness tends to get worse as the pressures of adult life increase. Adult symptoms of ADHD also tend to be far more subtle than childhood symptoms.
Some specialists have suggested the following as a list of symptoms associated with ADHD in adults:
• Impulsiveness
• Excessive activity or restlessness and edginess
• Carelessness and lack of attention to detail
• Continually starting new tasks before finishing old ones
• Poor organizational skills and problems prioritizing
• Poor time management skills
• Problems focusing on a task
• Poor planning
• Trouble multitasking
• Continually losing or misplacing things
• Forgetfulness
• Difficulty keeping quiet, and speaking out of turn
• Blurting out responses and often interrupting others
• Frequent mood swings, irritability, and a quick temper
• Low frustration tolerance
• Trouble coping with stress
• Extreme impatience
• Taking risks in activities, often with little or no regard for personal safety or the safety of others – for example, driving dangerously
Related conditions in adults with ADHD
Although ADHD doesn’t cause other psychological or developmental problems, as with ADHD in children and teenagers, ADHD in adults can occur alongside several related problems or conditions and make treatment more challenging.
• Mood disorders. Many adults with ADHD also have depression, bipolar disorder, or another mood disorder. While mood problems aren’t necessarily due directly to ADHD, a repeated pattern of failures and frustrations due to ADHD can worsen depression.
• Anxiety disorders. Anxiety disorders occur fairly often in adults with ADHD. Anxiety disorders may cause overwhelming worry, nervousness, and other symptoms. Anxiety can be made worse by the challenges and setbacks caused by ADHD.
• Learning disabilities. Adults with ADHD may score lower on academic testing than would be expected for their age, intelligence, and education. Learning disabilities can include problems with understanding and communicating.
• Other psychiatric disorders. Adults with ADHD are at increased risk of other psychiatric disorders, such as personality disorders, intermittent explosive disorder, and substance abuse.
– personality disorders – conditions in which an individual differs significantly from the average person in terms of how they think, perceive, feel, or relate to others
– bipolar disorder – a condition affecting your mood, which can swing from one extreme to another
– obsessive-compulsive disorder (OCD) – a condition that causes obsessive thoughts and compulsive behavior.
The behavioral problems associated with ADHD can also cause problems such as difficulties with relationships and social interaction.
The exact cause of attention deficit hyperactivity disorder (ADHD) is not fully understood, although a combination of factors is thought to be responsible.
Researchers suspect that a gene involved in the creation of dopamine, a chemical that controls the brain’s ability to maintain regular and consistent attention may be traced back to ADHD. ADHD tends to run in families and, in most cases, it’s thought the genes you inherit from your parents are a significant factor in developing the condition.
Research shows that parents and siblings of a child with ADHD are more likely to have ADHD themselves. However, the way ADHD is inherited is likely to be complex and is not thought to be related to a single genetic fault.
Among the factors that are thought to contribute to ADHD are:
• Brain injury or infection
• a lack of oxygen, or exposure to alcohol or nicotine before birth
• premature birth
• difficult experiences in early childhood.
ADHD SYMPTOM CHECKLISTS
Does My Child Have Attention Deficit Hyperactivity Disorder (ADHD or ADD)?
Only a mental health professional can tell for sure whether symptoms of distractibility, impulsivity, and hyperactivity are severe enough to suggest a positive ADHD diagnosis. ADHD Checklist for Boys and Girls tests may provide behavior clues and suggestions about the next steps. This questionnaire is designed to determine whether your child demonstrates symptoms similar to those of attention deficit disorder (ADHD). Download and print out the NICHQ Vanderbilt Assessment Scale. If you answer yes to a significant number of these questions, consult a licensed mental health practitioner. An accurate diagnosis can only be made through clinical evaluation.
Scoring Instructions for the NICHQ Vanderbilt Assessment Scales
These scales should NOT be used alone to make any diagnosis. You must take into consideration information from multiple sources. Scores of 2 or 3 on a single Symptom question reflect often-occurring behaviors. Scores of 4 or 5 on Performance questions reflect problems in performance.
The initial assessment scales, parent and teacher, have 2 components: symptom assessment and impairment in performance.
On both the parent and teacher initial scales, the symptom assessment screens for symptoms that meet the criteria for both inattentive (items 1–9) and hyperactive ADHD (items 10–18).
To meet DSM-IV criteria for the diagnosis, one must have at least 6 positive responses to either the inattentive 9 or hyperactive 9 core symptoms or both. A positive response is a 2 or 3 (often, very often) (you could draw a line straight down the page and count the positive answers in each subsegment). There is a place to record the number of positives in each subsegment, and a place for a total score for the first 18 symptoms (just add them up).
The initial scales also have symptom screens for 3 other comorbidities — oppositional-defiant, conduct, and anxiety/ depression. These are screened by the number of positive responses in each of the segments separated by the “squares.” The specific item sets and numbers of positives required for each co-morbid symptom screen set are detailed in the pdf file.
The second section of the scale has a set of performance measures, scored 1 to 5, with 4 and 5 being somewhat of a problem.
To meet the criteria for ADHD there must be at least one item of the Performance set in which the child scores a 4 or 5; ie, there must be impairment, not just symptoms to meet diagnostic criteria. The sheet has a place to record the number of positives (4s, 5s) and an Average Performance Score—add them up and divide by the amount of Performance criteria answered.
Adult ADHD Self-Report Scale (ASRS) Symptom Checklist
Many adults have been living with Adult Attention-Deficit/Hyperactivity Disorder (Adult ADHD) and don’t recognize it. Why? Because its symptoms are often mistaken for a stressful life. If you’ve felt this type of frustration most of your life, you may have Adult ADHD.
The following 6-question Adult Self-Report Scale-Version1.1 (ASRS-V1.1) Screener questionnaire can be used as a starting point to help you recognize the signs/symptoms of Adult ADHD but is not meant to replace consultation with a trained healthcare professional. An accurate diagnosis can only be made through a clinical evaluation. Regardless of the questionnaire results, if you have concerns about the diagnosis and treatment of Adult ADHD, please discuss your concerns with your physician.
The Adult Self-Report Scale Symptom Checklist is intended for people 18 or older.
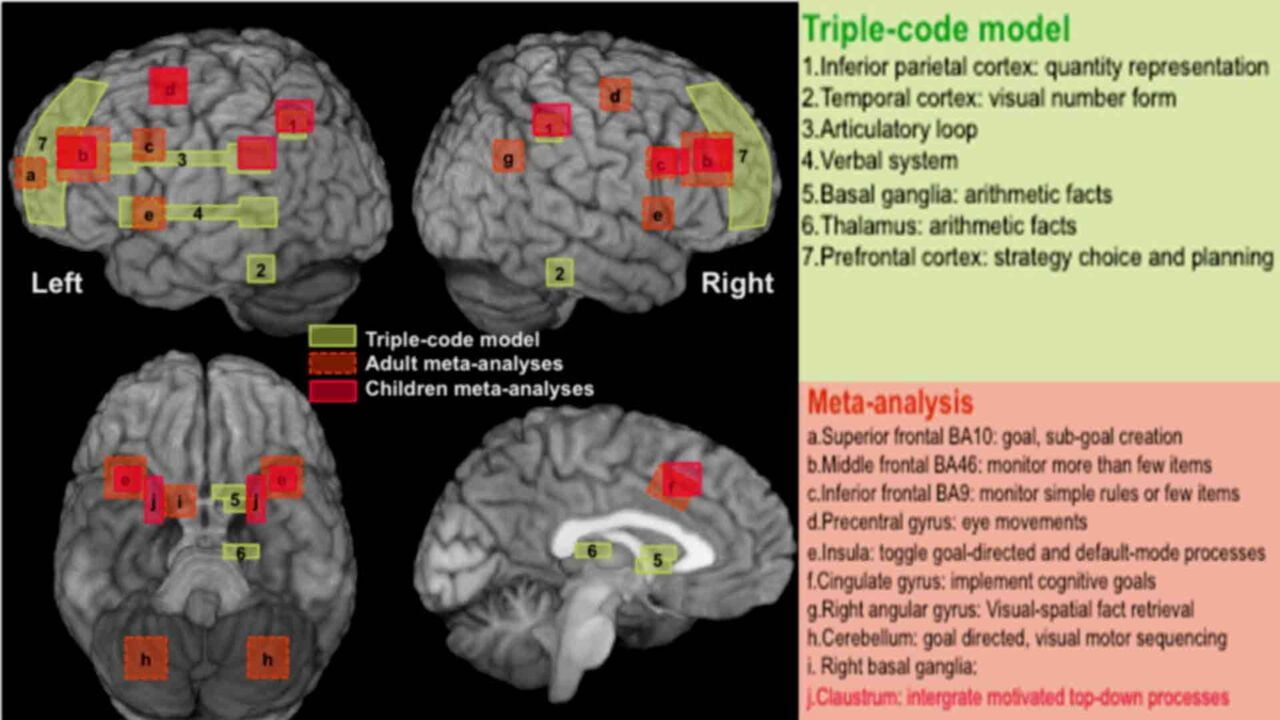
WHAT PARTS OF THE BRAIN ARE AFFECTED BY ADHD?
In children with ADHD, several brain regions and structures (pre-frontal cortex, striatum, basal ganglia, and cerebellum) tend to be smaller by roughly 5%.
ADHD brains have low levels of a neurotransmitter called norepinephrine. Norepinephrine is linked arm-in-arm with dopamine. The ADHD brain has impaired neurotransmitter activity in four functional regions of the brain.
1. Frontal Cortex
This region controls high-level functions:
• Attention
• Executive Function
• Organization
This region orchestrates our high-level functioning: maintaining attention, organization, and executive function. A deficiency of dopamine within this brain region might cause inattention, problems with organization, and/or impaired executive functioning.
2. Limbic System
This region is located deeper in the brain. It regulates our emotions and attention. A dopamine deficiency in this region might result in restlessness, inattention, or emotional volatility.
3. Basal Ganglia
These neural circuits regulate communication within the brain. Information from all regions of the brain enters the basal ganglia and is then relayed to the correct sites in the brain. A dopamine deficiency in the basal ganglia can cause inter-brain communication and information to “short-circuit,” resulting in inattention or impulsivity.
4. Reticular Activating System
This is the major relay system among the many pathways that enter and leave the brain. A dopamine deficiency here can cause inattention, impulsivity, or hyperactivity.
These four regions interact with one another, so a deficiency in one region may cause a problem in one or more of the others. ADHD results from problems in one or more of these regions.
NEUROPATHOPYSIOLOGY OF ADHD
The human brain consists of a million neurons secreting dopamine. The cells are scattered in different regions, and each area is responsible for different functions, including movement, cognitive functions, memory, and management skills such as decision-making and planning which enables attention and learning.
Dopamine is also secreted when feeling pleasure and success as part of positive feedback regulation. This miraculous system enables us to strengthen our desired behavior and progress in achieving our goals. The system works in the neural pathways that create a sense of pleasure, motivation, and concentration. When we have an interest or desire to succeed in the task, we secrete dopamine and the secretion of dopamine increases our motivation and attention and of course the feeling of success.
The reinforcement system operates under the mechanism of positive feedback, dopamine secretion is enhanced in response to success, and as a result, we are highly motivated and focused on the task.
ADHD is associated with several neurophysiological deficits. More recent theoretical approaches integrate clinical symptoms and neuropsychological difficulties within a framework of specific brain dysfunctions: cognitive deficits may emerge from dysfunctions particularly in fronto-striatal or mesocortical brain networks dopaminergic system, while problems with reward processing may be associated with dysfunctions in the mesolimbic dopaminergic system (Sagvolden et al., 2005; Sonuga-Barke, 2005).
However, deficits in ADHD may already be seen in the resting brain, and a more fundamental neuronal network approach suggests that in ADHD particularly Default Mode-Network (DMN) activity (usually prominent during rest) may interfere with activity in neuronal networks engaged in task processing, leading to difficulties in state regulation and periodic attentional lapses (Sonuga-Barke and Castellanos, 2007; Castellanos and Proal, 2012). That is why neurofeedback in ADHD management is very effective with long-lasting results.
Pharmacological interventions, particularly with stimulants such as methylphenidate and amphetamine sulfate, as well as non-stimulants like Atomoxetine, are highly effective in reducing ADHD symptoms (Banaschewski et al., 2006; King et al., 2006). What do ADHD medications do? In simple terms, they raise the level of norepinephrine within the brain. Stimulants work by causing the brain to synthesize more norepinephrine; non-stimulants by slowing the rate at which norepinephrine is broken down. Once the level is where it should be, the brain functions normally, and the individual becomes less hyperactive, inattentive, and/or impulsive. Once the drug wears off, the level falls — and symptoms return.
That’s because dopamine is hooked into the brain’s reward system. Having more dopamine circulating are feels like getting a bonus. It feels like that extra ten points on the test, right then. That means not only feel focused and content during the study but also to continue feeling that way. “The more you use it,” one student reported, “the more of it you want to use.”
The problem is that the good feelings, feeling in control and focused — these stop when the drug passes through your system a few hours later. The problem with drugs like Adderall and Ritalin is that you have to get more to feel better. That’s an addiction.
As report many researchers the long-term effectiveness is still questionable (Molina et al., 2009; van de Loo-Neus et al., 2011). In addition, side-effects, non-response, and prejudice have raised interest in non-pharmacological treatment options (Sonuga-Barke et al., 2013; Daley et al., 2014).
BRAIN WAVES IN ADHD
ADHD has been associated with certain clinical behavioral symptoms for many years. Recently, interest has been focused on ADHD, to determine whether certain abnormal EEG patterns correlate with clinical manifestations of ADHD.
Multiple studies have determined that compared to gender and age-matched controls, children with ADHD have greater theta activity. Other studies showed an increase in delta activity, coupled with decreased alpha and beta activities.
Additionally, abnormalities in the theta/beta ratio are one of the most significant measures of EEG alterations in ADHD.
Some researchers describe that in patients with ADHD theta/low beta ratio, and theta/alpha ratios were significantly increased.
Brain scans show that ADHD brains produce more low-frequency delta or theta brain waves than do neurotypical brains, and often show a shortage of the high-frequency beta brain waves linked to focus and impulse control.
NEUROFEEDBACK FOR ADHD MANAGEMENT
Neurofeedback (NFB) as a non-pharmacological intervention for ADHD management utilizes cognitive behavioral therapeutic elements to gain access to and practice brain activity. Several organizations worldwide are looking into claims that neurofeedback works just as well as pharma when it comes to helping kids with ADHD. A course of Neurofeedback sessions can have the same effect as the ongoing intake of psychostimulant medications like Ritalin, for example. The benefit of Neurofeedback, however, is that ongoing treatment is rarely needed after the course length and medications can be avoided altogether.
The functioning of the brain and a person’s behavior are connected. Changes in behavior can change the brain, and changes in the brain can change behavior. Neurofeedback aims to change a person’s behavior by changing their brain. With neurofeedback, it is possible to train the brain in a positive, natural way. The goal of neurofeedback is to increase the brain’s capacity for beta waves while diminishing the frequency of delta and theta waves.
Most recently, clinical trials have garnered interesting results attesting to both the presence of unique EEG patterns in the ADHD brain and the efficacy of theta suppression/beta enhancement and theta suppression/alpha enhancement protocols on ADHD symptoms reduction (see different NFB protocols detailed description on “NFB Protocol” page of this website, which will continuously update with the arrival of new research data).
In theta/beta training the goal is to decrease activity in the theta band (4–8 Hz) and to increase activity in the beta band (13–20 Hz) of the electroencephalogram (EEG) which corresponds to an alert and focused but relaxed state. Thus, this training paradigm addresses tonic aspects of cortical arousal. Alpha enhancement protocol was more effective in suppressing omission errors.
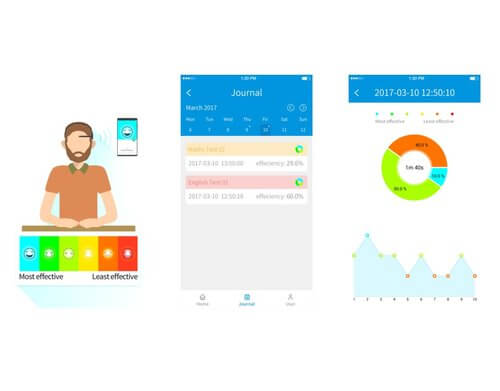
Practicing the neurofeedback allows the trainee to change his brainwave frequency to the desired frequency while using his self-regulation system. Today in the market there are a lot of Home Use Neurofeedback Headset Devices that can be used for home-based training and treatment. The neurofeedback trainee is wearing a headset that measures his brain frequency in real-time while he is playing a computer game that responds to the sensor (practically it responds to the user’s brain waves). Only when the NFB trainee’s brainwave frequency is as expected for attention or relaxation, he will score in the video game he is playing. When the trainee achieves points (meaning he has reached the desired frequency in the brainwaves), he experiences success the reinforcement system is activated and the excretion of dopamine increases naturally. The excreted dopamine increases attention and the trainee gets motivated to maintain the right frequency of the brainwaves. The flexibility of the brain is reflected in its ability to remember the way it changed frequency and by learning to reach the desired frequency even when the computer game is no longer there. This allows the trainee to keep the achieved attitude in everyday life and decrease symptoms of ADHD.
Neurofeedback has been introduced to treat ADHD and can improve attention levels and alleviate hyperactivity symptoms. The process provides a mechanism by which the patient can normalize the cortical activity profile by decreasing slow-wave activity and increasing fast-wave activity. It is expected that compensation of the dysfunctional electroencephalogram (EEG) enhances concentration and attention and increases the arousal level. Patients will learn how to enhance the desirable EEG frequencies associated with relaxed attention and how to reduce the undesirable frequencies that are associated with under- or over-arousal.
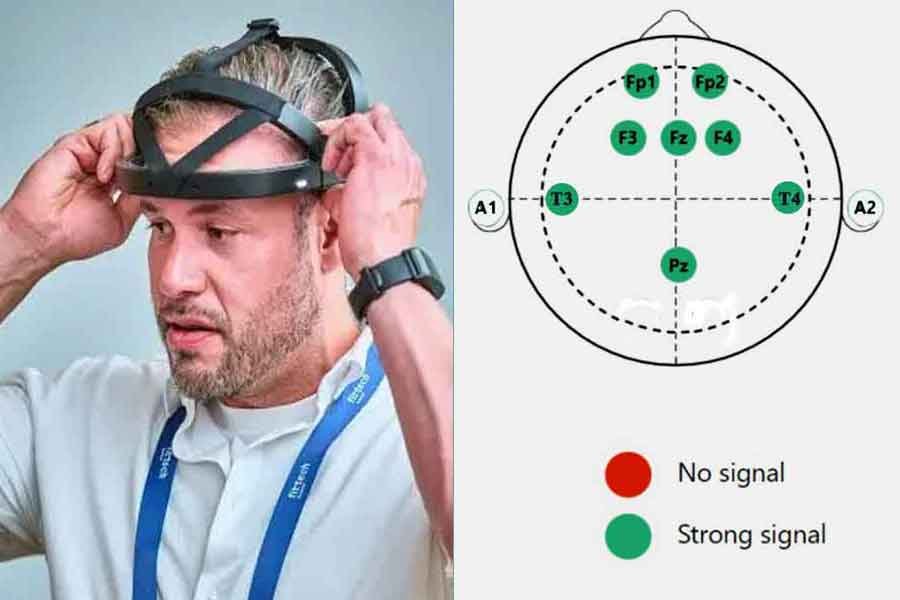
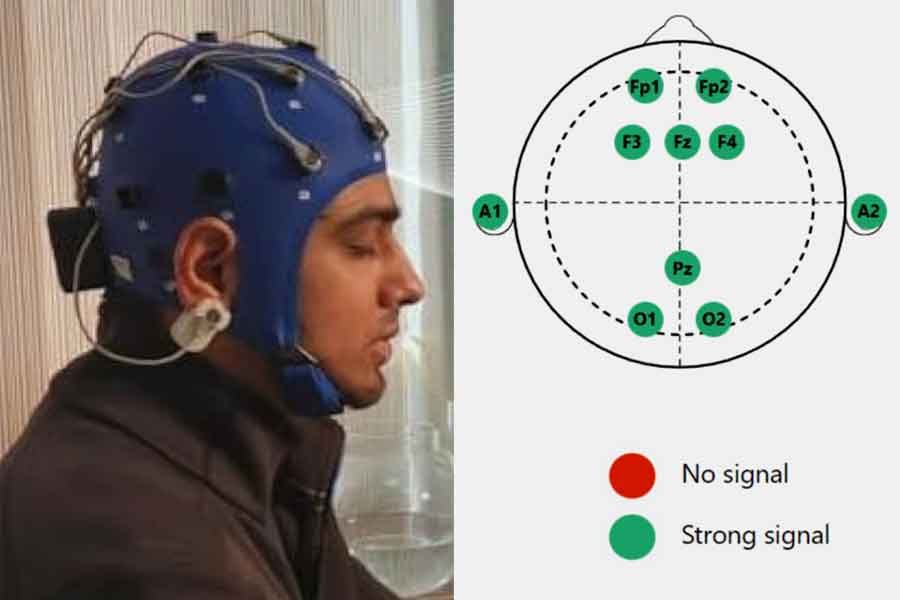
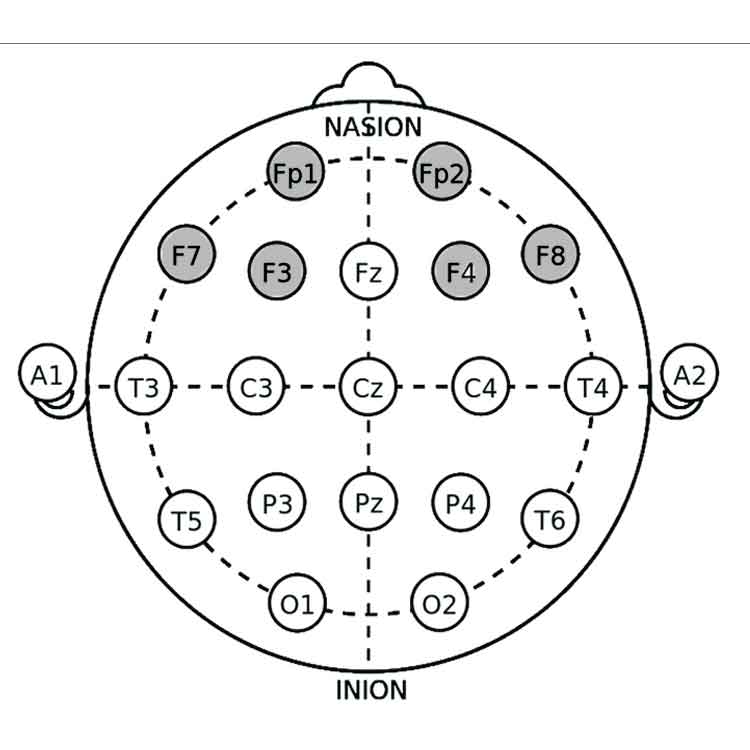
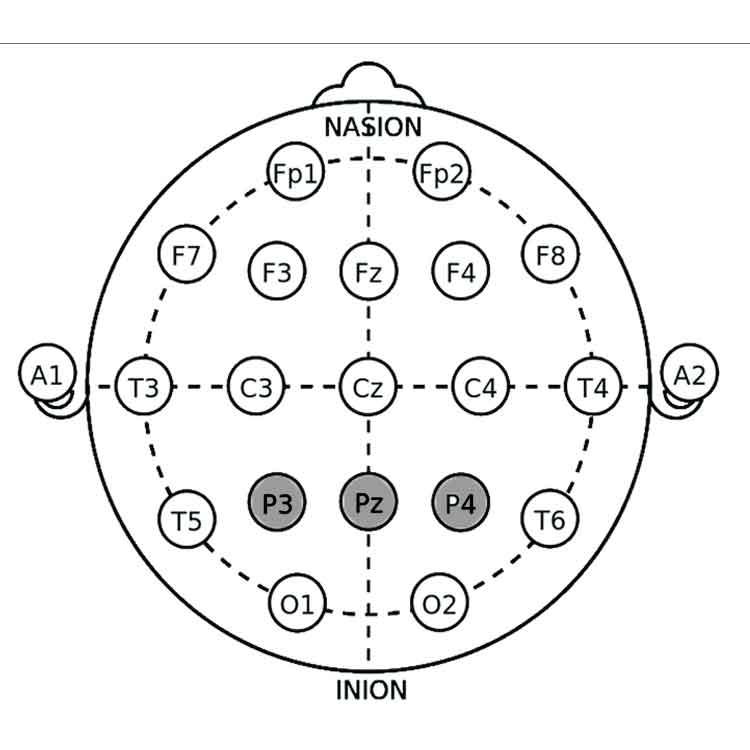
Key Electrode Sites for ADHD Neurofeedback
1. Fz (Frontal Midline):
• Location: Frontal lobe, on the midline, 20% of the distance from the nasion (bridge of the nose).
• Relevance: Associated with attention, impulse control, and executive function. Targeting Fz can help improve these areas.
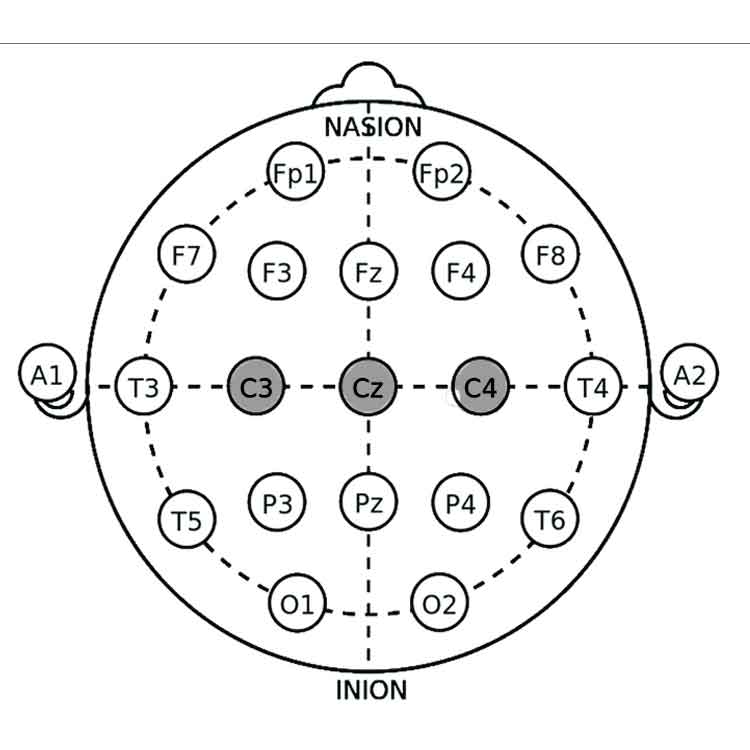
2. Cz (Central Midline):
• Location: The scalp vertex, halfway between the nasion and inion and equally spaced between the left and right preauricular points (just above the ears).
• Relevance: Central region involved in motor control and general arousal regulation. Often used as a reference site.
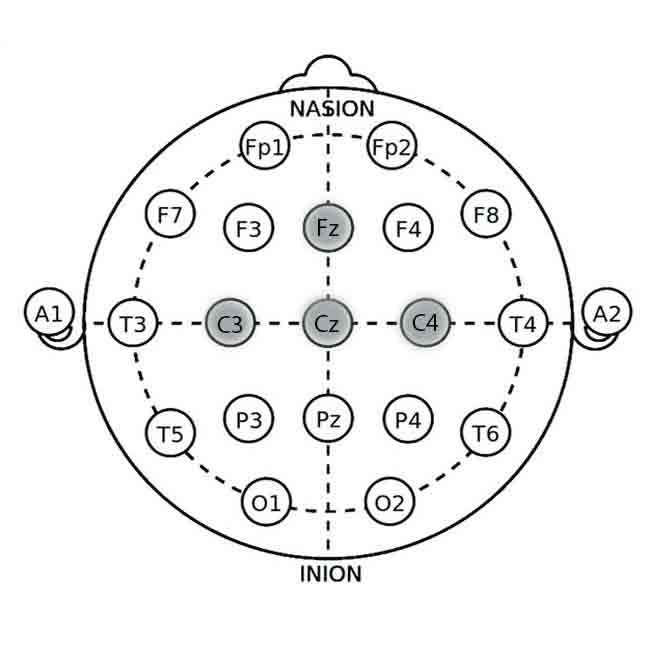
3. C3 (Left Sensorimotor Cortex):
• Location: Left hemisphere, 20% of the distance from the midline along the central line.
• Relevance: Involved in motor control and coordination, relevant for reducing hyperactivity.
4. C4 (Right Sensorimotor Cortex):
• Location: Right hemisphere, analogous to C3 on the right side.
• Relevance: Also involved in motor control; balancing neural activity related to motor functions.
Neurofeedback Protocols for ADHD Management
The protocol involves training individuals to increase or decrease specific brainwave activity at the targeted locations to improve attention, impulse control, and executive function.
1. Theta/Beta Ratio Training
This protocol aims to balance theta (4-8 Hz) and beta (15-20 Hz) wave activity to improve attention and reduce impulsivity.
• Target Brainwaves: Theta (4-8 Hz) and Beta (15-20 Hz)
• Goal: Decrease theta activity and increase beta activity to improve cognitive control and reduce symptoms of ADHD.
Procedure:
1. Electrode Placement: Place electrodes at Fz and Cz (reference).
2. Baseline Recording: Record baseline theta and beta activity for 5-10 minutes.
3. Feedback Mechanism: Provide real-time feedback using visual (e.g., a game or moving bar) or auditory (e.g., tone) cues. Positive feedback occurs when theta decreases and beta increases.
4. Training Sessions: Conduct sessions for 20-30 minutes, 2-3 times per week, for 20-40 sessions.
5. Progress Monitoring: Utilize attention and impulse control scales along with follow-up qEEG to track progress.
2. SMR Training Protocol
This protocol focuses on increasing sensorimotor rhythm (SMR, 12-15 Hz) activity to enhance motor inhibition and reduce hyperactivity.
• Target Brainwaves: SMR (12-15 Hz)
• Goal: Increase SMR activity to enhance motor inhibition and promote calmness.
Procedure:
1. Electrode Placement: Place electrodes at C3 (left sensorimotor cortex) and Cz (reference).
2. Baseline Recording: Record baseline SMR activity for 5-10 minutes.
3. Feedback Mechanism: Provide real-time feedback using visual or auditory cues. Positive feedback is given when SMR activity increases.
4. Training Sessions: Conduct sessions for 20-30 minutes, 2-3 times per week, for 20-40 sessions.
5. Progress Monitoring: Use attention and hyperactivity rating scales and follow-up qEEG to monitor changes.
3. Alpha/Theta Training
This protocol focuses on balancing alpha (8-12 Hz) and theta (4-8 Hz) waves to promote relaxation and improve cognitive control.
• Target Brainwaves: Alpha waves (8-12 Hz) and Theta waves (4-8 Hz)
• Goal: Increase alpha activity and decrease theta activity to enhance relaxation and attention.
Procedure:
1. Electrode Placement: Place electrodes at Fz and Cz (reference).
2. Baseline Recording: Record baseline alpha and theta activity for 5-10 minutes.
3. Feedback Mechanism: Use calming visual or auditory feedback. Positive feedback is provided when alpha increases and theta decreases.
4. Training Sessions: Conduct sessions for 20-30 minutes, 2-3 times per week, for 20-40 sessions.
5. Progress Monitoring: Use attention and relaxation scales along with follow-up qEEG to monitor changes.
Effectiveness of Neurofeedback for ADHD management
Moreover, long-term follow-up studies with children successfully treated with neurofeedback have shown that the improved attention ability and memory improvement of these children remain stable long after treatment has ended. These children also learn easier manage their emotional status in different stressful situations. In other words, abnormal brainwave patterns are permanently normalized without the use of toxic drugs. It is also important to note that drugs do not improve the child’s ability to learn but neurofeedback does.
The research shows that neurofeedback works best for children over 6 years of age with normal or high intelligence. Usually, some 30-50 treatment sessions (30-45 minutes each) are required for successful treatment, at a rate of 2-3 sessions per week.
After 1-5 sessions
After 6-10 sessions
After 11-20 sessions
After 20+ sessions
HOME USE DEVICE FOR NEUROFEEDBACK FOR ADHD MANAGEMENT
Neurofeedback devices and systems are used for both medical and non-medical uses, and the dividing line between them may be thin. Non-medical application of neurofeedback can be considered primarily as personal improvement and conditioning for the brain and mind: to improve relaxation, attention, focus, concentration, and self-awareness, or as an adjunct to meditation, counseling, hypnosis, or achieving altered states of consciousness. It can be done without professional intervention. In cases where it is desired to relieve the conditions of a medical problem, professional help should be sought.
It is a fact that Neurofeedback systems are designed to allow the user to control a computer for recreational, educational, or entertainment purposes and are not medical instruments. You can find detailed information regarding indications, methods, and descriptions of different neurofeedback devices for home use here. However, if direct benefits are claimed for relaxation or relief from the symptoms of disorders, then the device is considered medical.
In the nonclinical embodiment, most of the same functions and capabilities are present, but they are presented in the context of an educational and recreational device. It is nonetheless true that the actual benefits may be essentially the same in both embodiments depending on how the user configures and applies the device, although the labeling and claims are different. The same instrument is being provided in both cases but with different intent.
The difference between the medical and non-medical embodiment of NFB devices lies primarily in the claims and the expectations and applications of the user.
For example, although neurofeedback can be used to improve attention and concentration, and this can be considered a personal improvement application, in cases of suspected or diagnosed Attention Deficit Hyperactivity Disorders the use of this procedure might be regarded as a medical procedure.
It may thus be argued that neurofeedback treatment intended to reduce the symptoms of ADHD, especially when the removal from stimulants (Ritalin, etc) is desired, that neurofeedback is being used in a medical context. However, if a parent, teacher, or counselor uses neurofeedback in a home or educational setting to educate a child on how to reach a state of relaxed attentiveness and improve academic success, the treatment may be considered education, not treatment.
Neurofeedback takes advantage of the brain’s ability to change itself through a process known as Neuroplasticity. It utilizes the same learning process that occurs whenever we acquire a new skill. The brain learns by forming connections between nerve cells and utilizing important pathways that connect different locations in the brain.
The more frequently you utilize these pathways the better the brain becomes at performing the associated task.
This type of learning is a type in which responses come to be controlled by their consequences. Quite simply, Neurofeedback offers the perfect learning conditions, since it facilitates awareness of when the brain is producing healthier brainwave patterns, reinforces the positive change, and multiple opportunities to provide practice during a training session.

Excellent Brain ADHD Neurofeedback Home Training Kit




Neurosky Puzzlebox Orbit Bundle EEG Headset
Biofeedback Home Use Device
Various modalities of biofeedback, including Electromyography (EMG), Heart Rate Variability (HRV), Temperature, and Galvanic Skin Response (GSR), can also be utilized in the management of Attention-Deficit/Hyperactivity Disorder (ADHD). EMG biofeedback helps individuals gain awareness and control over muscle tension, which can reduce physical restlessness and hyperactivity often associated with ADHD. HRV biofeedback trains individuals to regulate their heart rate variability, promoting autonomic balance and improving emotional regulation and stress resilience. Temperature biofeedback involves monitoring peripheral skin temperature to enhance relaxation and decrease physiological arousal, thereby aiding concentration and impulse control. GSR biofeedback measures the electrical conductance of the skin, which varies with sweat gland activity and can provide insights into stress and arousal levels. By learning to modulate these physiological responses, individuals with ADHD can improve their focus, reduce impulsivity, and manage stress more effectively, complementing traditional neurofeedback approaches.
EMG Biofeedback home-use device
Temperature Biofeedback home-use device
Electrodermal Skin Activity Biofeedback home-use device
ADHD OTHER MANAGEMENT MEANS
DIET AND NATURAL SUPPLEMENT IN ADHD
• Proteins
• Balanced Meals
• B Vitamins
• Zinc, Iron, and Magnesium
• Multivitamins/ Multimineral
• Picamilon
• Proteins
Foods rich in protein: lean beef, pork, poultry, fish, eggs, beans, nuts, soy, and low-fat dairy products — can have beneficial effects on ADHD symptoms. Protein-rich foods are used by the body to make neurotransmitters, the chemicals released by brain cells to communicate with each other. Protein can prevent surges in blood sugar, which increases hyperactivity.
• Balanced Meals
A well-balanced diet, including vegetables, complex carbohydrates, fruits, and plenty of protein, leads to behavior that tends to be more consistently under control.
• B Vitamins
Studies suggest that B vitamin supplements may improve IQ scores and reduce aggression and antisocial behavior in children who are B-vitamin deficient. Vitamin B-6 may also increase the brains’
levels of dopamine, a neurotransmitter that improves alertness.
• Zinc, Iron, and Magnesium
Zinc synthesizes dopamine and boosts the effects of some ADHD stimulant medications, such as Ritalin and Concerta; low levels of zinc correlate with inattention. Iron is also necessary for making dopamine; low levels of iron may cause cognitive deficits and severe ADHD. Adequate levels of magnesium keep the brain calm
• Multivitamins/Multiminerals
Daily recommended a value of vitamins and minerals are important for any child, especially one with ADHD. A daily multivitamin/multimineral will ensure that he gets what he needs.
• Picamilon
A combination of the B-vitamin niacin and gamma-aminobutyric acid, picamilon improves blood flow to the brain. It’s been shown to improve alertness and attention, as well as reduce aggressive behavior.
OMEGA 3 IN ADHD MANAGEMENT
It is rapidly becoming acknowledged that omega-3 fatty acids are good for the brain. Our requirements for EPA (Eicosapentaenoic Acid) and DHA (Docosahexaenoic Acid) change throughout life and so does the optimal amount of each fatty acid in our diet.
Children require DHA for growth and development, and the brain, CNS, and retina rely heavily on the adequate supply of DHA during growth in the womb.
Children continue to need DHA up until the age they start school, so if children under the age of five are taking an omega-3 supplement, it should contain DHA.
After the age of five, the development of the brain and CNS starts to reduce and the body’s need for DHA reduces. This is a good time to increase EPA in the diet, as studies show that EPA can help with childhood behavior and academic performance, as well as focus, attention, and reducing aggression.
Research has shown that EPA levels are under constant demand and low EPA levels in adolescents and adults correlate strongly with the development of mental health issues, including depression, dyslexia and dyspraxia, heart problems, joint and bone conditions, as well as neurodegenerative diseases such as MS and Parkinson’s.
The majority of the body’s needs can be met by using EPA-rich oils and eating fish, marine products, organic greens, and pastured animal products.
Recent studies suggest that ADHD children may be deficient in omega-3 and that a daily supplement may decrease ADHD symptoms while improving focus and cognitive function.
Studies have yet to determine an optimum dosage of omega-3, or fish oil, in children or adults with attention deficit hyperactivity disorder (ADHD). It is recommended that children four to six years of age start with a daily supplement of 500 mg of omega-3; for children seven years and older, 1000 mg.
It is determined that supplements with an EPA: DHA ratio of 2:1 with Vitamin E are the more effective for ADHD management (85% effectiveness with extension of effect over the following 6 months). Such a supplement is eVitamins Ultra Omega 3 – 750 mg with EPA/DHA – 500/ 250 that is very effective for the management of ADHD symptoms.
SPORT IN ADHD MANAGEMENT
Thirty minutes to a full hour of physical activity per day can make a huge difference in anyone’s mental and physical health, but especially for a child with ADHD. A child with ADHD who is regularly active may sleep better and experience fewer emotional outbursts at home and school. They may see benefits from the structure and organization of being part of a team and learning the rules of a new game or activity. Kids can also learn communication and social skills, increase coordination skills, and build up their self-esteem by being part of a sport or other activity. Because people with ADHD are at increased risk for developing depression, activities that involve exercise can lower their risk for depressive symptoms.
Sports offer lots of social interaction in addition to physical fitness. This helps kids with ADHD bond with their peers, and it helps get them out of their shell. A common issue with ADHD kids is to find something to help them gain confidence and self-esteem. They can use sports as a vehicle for making and having friends. Healthy activities like sports are better than sitting alone or in front of the television.
How do you know what sport will be best for your child? Ask him what he wants to do. Always support the choices and decisions of your child, because if he chooses to do something because he likes it then he will do it right and have a great time with it.
Many kids will see or try a lot of different athletic activities, whether at school, during camp, or in after-school programs. That gives them the chance to decide what appeals the most.
These are the best after-school activities for kids with ADHD: Swimming, Track and Cross-country, Horseback riding, Tennis, Baseball, Basketball, Gymnastics, Martial arts, Soccer, Wrestling, Archery, etc.
It’s important to remember that it might take several tries before your child finds the right sport or activity for them. It may be too much to try multiple things at once, so consider trying different sports or activities in different seasons and then letting your child decide what they like best. Never underestimate your child’s abilities because they have ADHD.
Many successful athletes like Michael Phelps, Simone Biles, Michael Jordan, and Terry Bradshaw have shared their experiences with the disorder. Artists like actor Jim Carrey, musician Adam Levine, and writer Jenny Lawson have gone on to create inspiring things while living with an ADHD diagnosis.